Nearly 10% of women experience pruritus vulvae, an inflammatory condition of the external female genitalia characterized by persistent itching, redness, or skin thickening. This manifestation often stems from various triggers such as hormonal shifts during menopause, allergic reactions to hygiene products, or underlying dermatological conditions like lichen sclerosus.
Persistent irritation frequently disrupts daily activities and sleep, yet many individuals delay seeking professional advice due to the sensitive nature of the symptoms. This article clarifies the primary causes of vulvar discomfort and provides practical strategies for effective long term skin management.
- Identifying the Causes of Vulvar Itching and Discomfort
- Clinical Evaluation and Long-Term Skin Management
- At-Home Strategies for Irritation Prevention
- Timelines for Seeking Professional Intervention
Identifying the Causes of Vulvar Itching and Discomfort
Vulvar itching, or pruritus vulvae, affects nearly 10% of women, often stemming from non-infectious irritants, hormonal shifts during menopause, or conditions like lichen sclerosus rather than simple yeast infections. Understanding anatomical boundaries is the first step.
Pruritus vulvae: Inflammation or itching of the vulva, the external female genitalia, affecting roughly 10% of women.
Differentiating Between Vulvar and Internal Vaginal Issues
The vulva constitutes the external skin, while the vaginal canal remains internal. These areas possess distinct skin barriers. Sensory receptors on the vulva react differently than those within internal tissues.
External itching involves localized skin irritation. This differs from internal symptoms like unusual discharge. Such distinctions help identify this common and distressing condition accurately without confusion.
External Irritants and Infectious Agents
Harsh soaps and scented detergents often disrupt the protective skin barrier. Synthetic fabrics can trigger an inflammatory response. Dyes and fragrances act as common culprits for persistent redness.
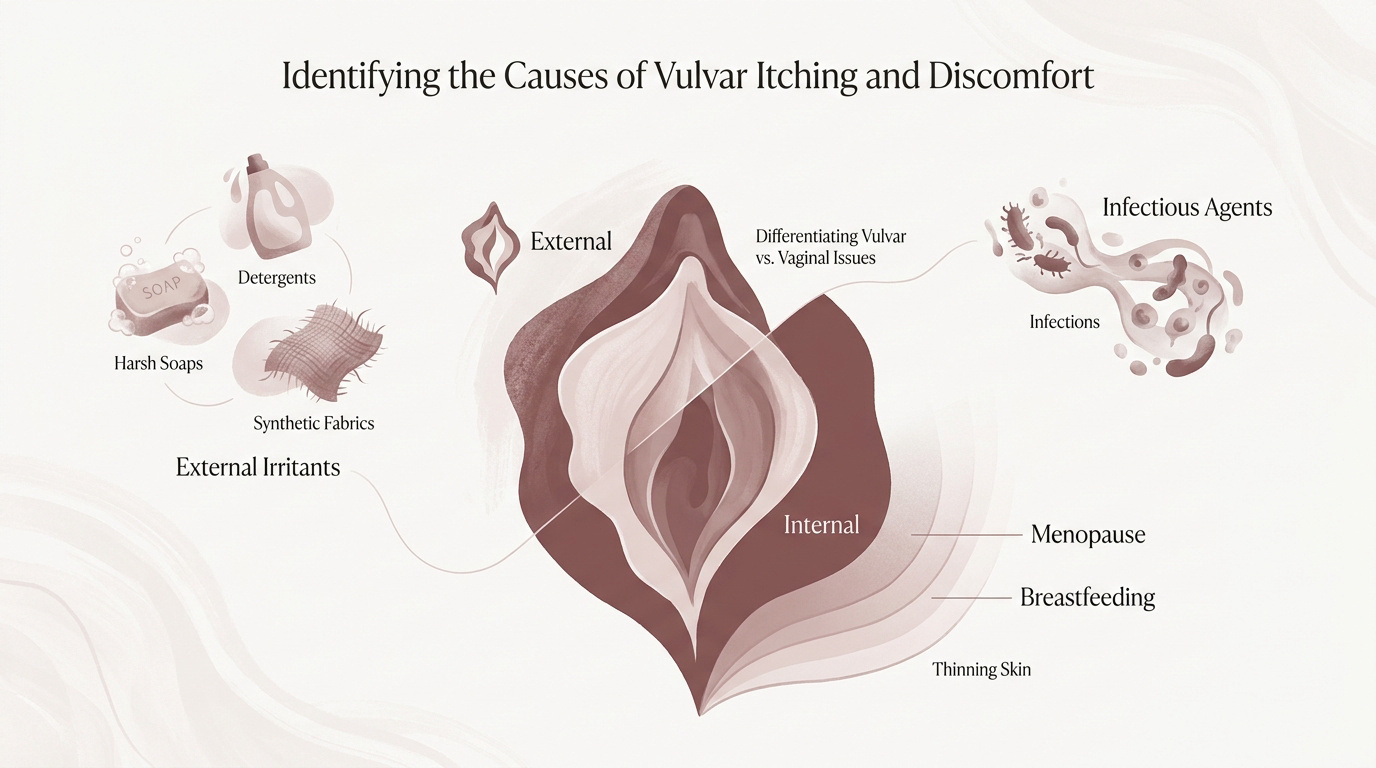
Bacterial vaginosis and STIs serve as infectious triggers. These pathogens alter local pH levels, causing persistent itching. Common irritants include soaps, detergents, and synthetic underwear.
Impact of Menopause and Breastfeeding on Skin Integrity
Falling estrogen levels during menopause lead to thinning of vulvar tissue. This atrophy reduces natural moisture and elasticity. The skin becomes increasingly fragile and prone to discomfort.
Breastfeeding also induces a low-estrogen state. This change mimics symptoms of the genitourinary syndrome of menopause. It leaves the skin susceptible to micro-tears and chronic irritation during daily activities.
Clinical Evaluation and Long-Term Skin Management
While home observations are helpful, clinical diagnostics provide the necessary clarity for persistent symptoms that don’t resolve with basic care.
Understanding the Diagnostic Exam and Biopsy Procedures
The pelvic exam process is straightforward. A professional uses swabs to rule out yeast or bacteria. Visual inspection remains the primary diagnostic tool.
Skin biopsies target suspicious lesions specifically. This small sample identifies the exact dermatological disease. It ensures the treatment matches the actual pathology found.
Recognizing Lichen Sclerosus and Chronic Inflammation
Lichen sclerosus and lichen simplex chronicus cause white, thin patches or thickened skin. These are chronic conditions. They require consistent medical supervision to prevent scarring. Experts focus on managing common vulvar skin conditions through specialized protocols.
Long-term monitoring is vital for health. Specialized care prevents complications like structural changes or rare malignancies.
Scratching damages the skin barrier, leading to secondary infections, chronic pain, or permanent skin changes like thickening.
Investigating Nocturnal Itching and Sleep Disruption
Itching often intensifies at night. This happens due to lack of distractions and natural temperature fluctuations. Evening cortisol drops also play a role.
The “itch-scratch cycle” is a serious issue. Scratching during sleep damages the skin barrier further. This creates inflammation and prevents tissue from healing properly.
At-Home Strategies for Irritation Prevention
Beyond clinical treatments, managing your daily environment is the most effective way to break the cycle of chronic vulvar sensitivity.
Daily Hygiene Protocols and Fabric Selection
Wash the area using only plain water or soap-free cleansers. Avoid douching or internal cleaning. Gently pat the skin dry with a soft towel.

Choose breathable 100% cotton underwear. Loose clothing reduces friction and heat. This prevents moisture buildup that encourages fungal growth or skin maceration.
Pitfalls of Inappropriate Over-the-Counter Treatments
Avoid antifungal creams without a diagnosis. These can cause contact dermatitis if no infection exists. Steroid creams may thin skin if used incorrectly. Self-diagnosis often delays professional help.
Using random creams risks masking serious symptoms. This changes the skin’s appearance, making clinical diagnosis harder.
Managing Sensitivity Related to Lifestyle and Exercise
Blood sugar management is linked to recurrent infections. High glucose levels fuel yeast growth. This is vital for those with poorly controlled diabetes.
Shower immediately after swimming or cycling. Use a barrier balm to protect skin from sweat and friction. This maintains the skin barrier during physical movement.
| Activity | Risk Factor | Prevention Strategy |
|---|---|---|
| Swimming | Chlorine/Dampness | Rinse and change immediately |
| Cycling | Friction | Use barrier balm |
| Running | Sweat | Wear breathable cotton |
| Gym | Tight synthetics | Shower and change post-workout |
Persistent symptoms like pruritus vulvae require professional attention. Proper hygiene and clothing choices are powerful tools for long-term comfort and skin health.
Timelines for Seeking Professional Intervention
Knowing when to stop home remedies and seek an expert opinion can prevent long-term damage and provide much-needed peace of mind.
Identifying Abnormal Skin Changes and Color Shifts
Regular self-exams using a handheld mirror are highly effective for monitoring health. Look for new bumps, sores, or persistent red patches. Note any changes in skin texture or thickness.
Color shifts toward white or dark brown require professional attention. These can indicate chronic inflammatory states or early cellular changes. Early detection is key for effective management.
Monitor any moles in the genital area. Report asymmetrical shapes or changing borders to a provider.
- Persistent redness
- White patches
- New lumps or bumps
- Open sores that don’t heal
Seek medical advice if pruritus vulvae symptoms last over 2 weeks, or if you notice persistent redness, white patches, new lumps, or bleeding.
When to Transition from Home Care to Clinical Diagnosis
Set a strict timeframe for home care. If symptoms persist beyond two weeks of avoiding irritants, see a doctor. Immediate consultation is necessary if pain or bleeding occurs. Professional help is vital for non-infectious issues that don’t respond to basic hygiene.
Dermatologists play a critical role in diagnosis. They specialize in complex skin conditions that general practitioners might overlook during a standard exam.

Specialized clinics offer targeted biopsies. These tests provide a definitive roadmap for long-term relief.
Managing pruritus vulvae requires identifying irritants, stabilizing the skin barrier, and seeking clinical diagnostics for persistent symptoms. Transition to breathable fabrics and medical evaluation now to prevent chronic inflammation. Proper care ensures a future of lasting comfort and restored skin integrity.
